

Interventional pulmonology
Interventional pulmonology is a relatively novel field in chest medicine. In our hospital, the members in this field include pulmonologists and chest surgeons who can perform advanced diagnosis and treatment technology for lung disease. The combination of bronchoscopic, transthoracic, and surgical techniques helps achieve the special and integrated features of interventional pulmonology.
We performed invasive procedures, including bronchoscopy-guided lung biopsy, transbronchial needle aspiration, transbronchial ablation, pleuroscopy, bronchoscopic trans-parenchymal nodule access (BTPNA), bronchoscopic thermal vapor ablation (BTVA), iGuided transthoracic lung biopsy, and transthoracic microwave or cryoablation. In our hospital, we can perform a “one stop” procedure for lung nodules, including tumor localization via bronchoscopy or transthoracic localization followed by thoracic surgical procedure.
Using the “one stop” method, we could avoid the time lag between localization and surgical resection; besides, we can also prevent the possible complications during patient transferal. We performed bronchoscopy biopsy, including forcep biopsy and cryobiopsy. Many procedures were performed under the guidance of augmented fluoroscopy.
The localization under augmented fluoroscopy increased the yield rate of tissue proof, especially in the relative peripheral lung lesion. We also performed many transthoracic needle aspirations from mediastinal lesions. We performed transthoracic biopsy and microwave or cryoprobe ablation with iGuide assistance under augmented fluoroscopy guidance.
We often performed the procedure with the patient under general anesthesia. In our institute, we can manage the lung lesion or obtain the lung tissue via multimodal methods. These methods need cooperation between the pulmonologist and the chest surgeon and provide more precise treatment and diagnosis for patients with lung disease.
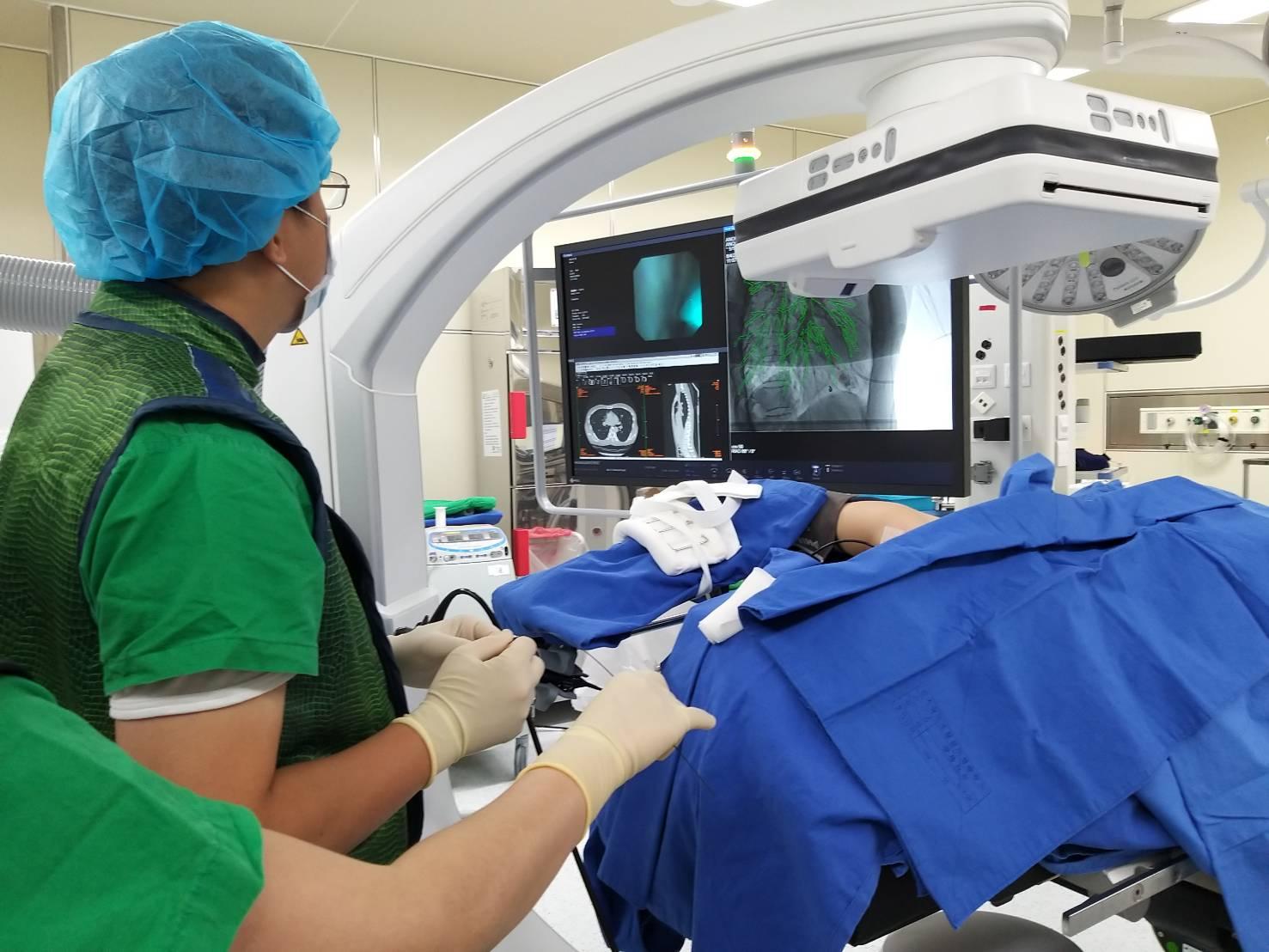
Benefits of the procedure:
Thoracic surgery can remove the lesions within the chest. The benefits and likelihood of successful treatment vary depending on the type of surgery, and some examples are as follows:
Thoracic surgery for pneumothorax is expected to reduce recurrence rate by 20%.;
Thoracic surgery for early-stage lung cancer can achieve a 5-year survival rate of up to 90%.;
Esophageal cancer surgery performed with thoracoscopy can increase the postoperative extubation success rate to 90%.
Risks of the procedure:
Surgical Risks: Complications and unexpected situations that may occur during or after surgery.
Anesthesia:
General anesthesia will be administered during the surgery, and postoperative pain management will involve self-controlled analgesia or oral and injectable pain medication. Common anesthesia-related issues include nausea, vomiting, generalized soreness, throat discomfort, and hoarseness. Occasionally, dental and lip injuries may occur. Severe complications such as respiratory distress, stroke, or myocardial infarction are rare and typically occur in patients with poor preoperative lung function, advanced age, obesity, smoking, heart disease, diabetes, kidney disease, hypertension, and other significant medical conditions.
General surgical risks:
Some complications can occur in all types of surgeries, including thoracic surgery. These complications may include lung infections, deep vein thrombosis with a small risk of pulmonary embolism, and insufficient blood flow leading to stroke or cardiac ischemia.
Specific risks associated with thoracic surgery may include: